Mohs micrographic surgery is one of the most effective methods for treating skin cancer. The technique carefully removes the entire tumor without harming any surrounding tissue by taking a precise, layer-by-layer approach. To learn how to perform Mohs surgery, physicians study under the guidance of a Mohs College member for a year after completing a traditional three-year dermatology residency. Compared to other skin cancer treatments, Mohs surgery has one of the highest success rates, up to 99 percent, largely due to the intense training Mohs specialists receive. Mohs surgery minimizes scarring, since it avoids the removal of healthy tissue and precisely targets all cancerous areas. In addition, physicians perform the technique using only local anesthetic, so it can be performed as an outpatient procedure, making it a quick and cost-effective surgery compared to other treatments.
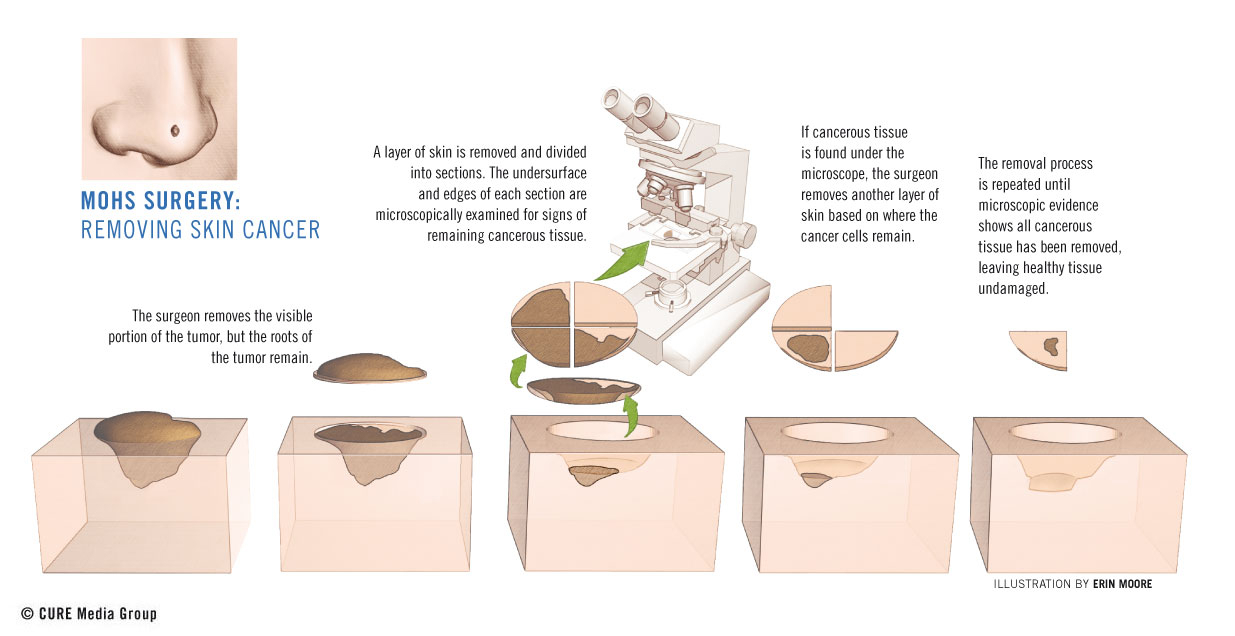
During Mohs surgery, the physician removes the visible portion of the skin tumor and analyzes the tissue under a microscope, creating a map of healthy and cancerous cells. Using this graphic aid, the physician removes another thin layer of cancerous cells, retaining any healthy layers of skin. With each removal, the physician carefully analyzes the tissue for remaining cancer cells and continues with the procedure until no evidence of cancerous cells remains. Physicians examine all surfaces of the removed tissue to ensure that the entire tumor has been excised. By proceeding one layer at a time, the dermatologist avoids damaging or removing cells unnecessarily while guaranteeing complete eradication.
Mohs surgery effectively treats cancers that affect large areas of skin and those without clearly defined boundaries. Dermatologists also recommend the procedure for cancers on the face, ears, and neck, to produce the most cosmetically appealing results and when another treatment has failed and the cancer has returned. Physicians most often use Mohs surgery to treat aggressive cancers, such as basal cell carcinoma, squamous cell carcinoma, sebaceous carcinoma, and extramammary Paget’s disease.